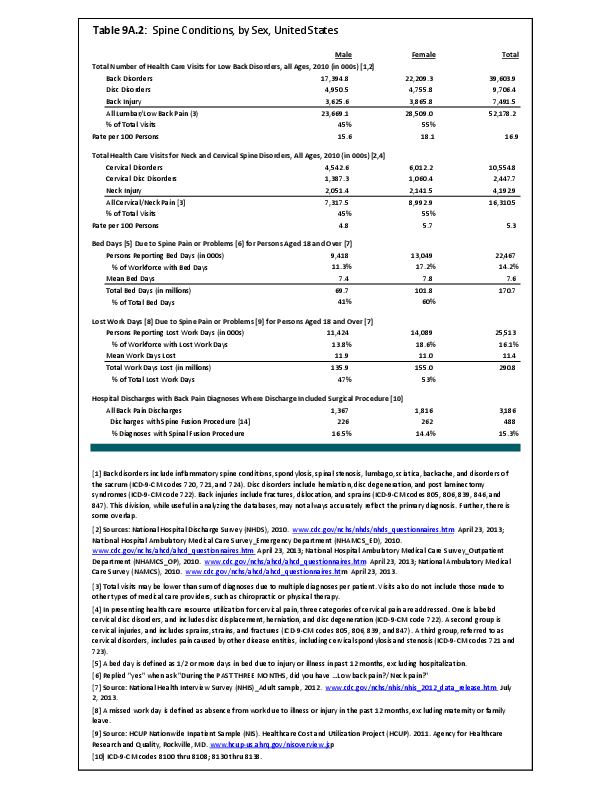
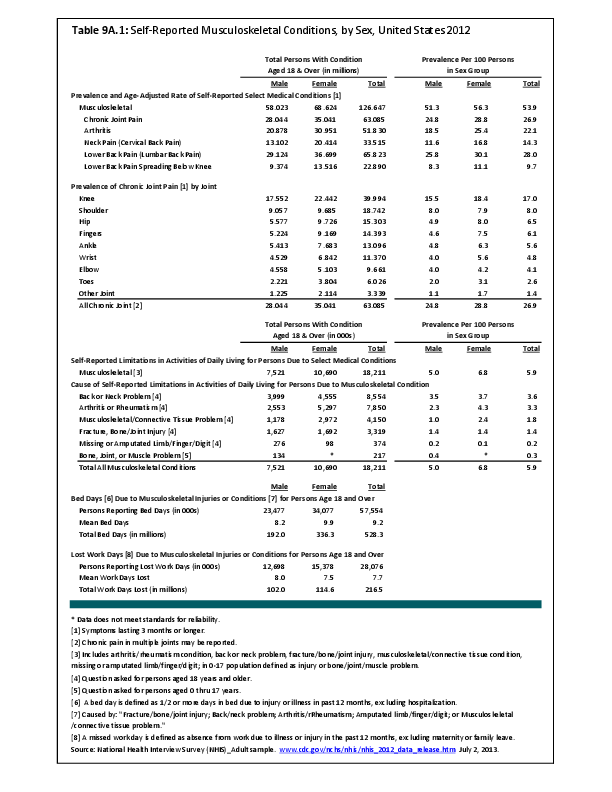
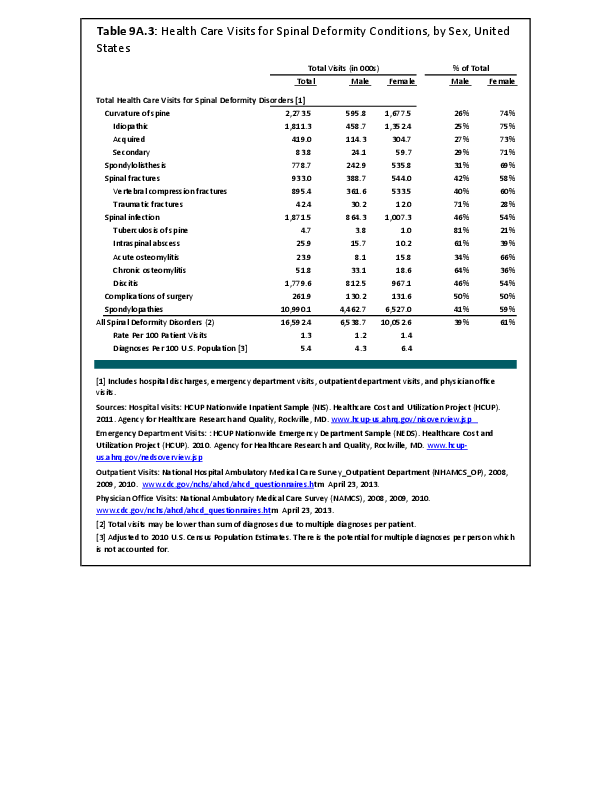
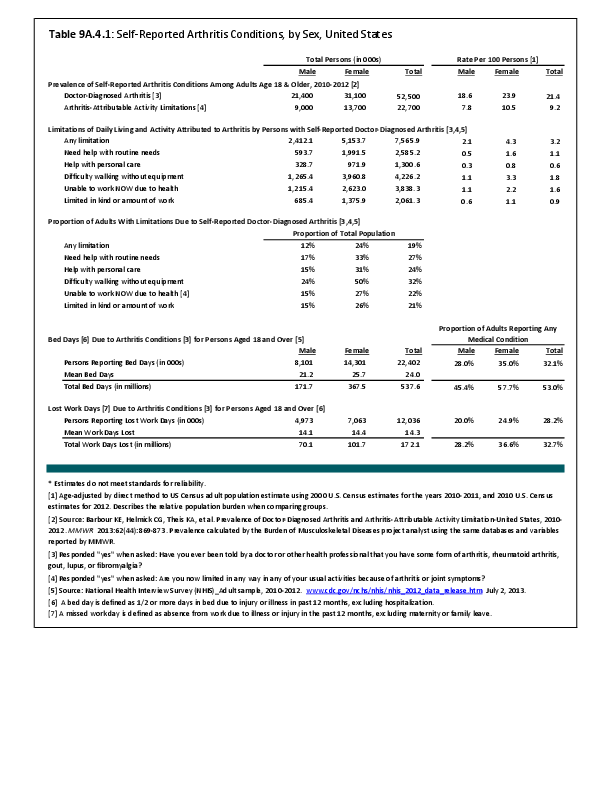
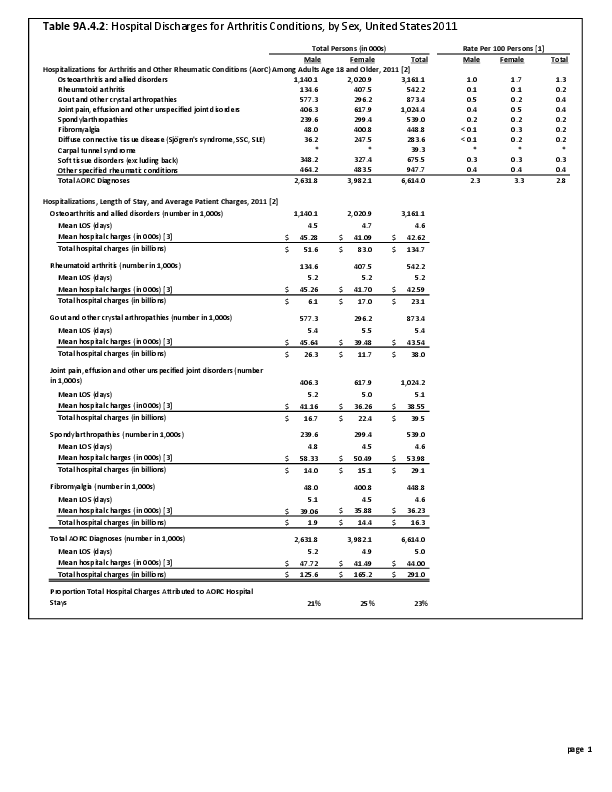
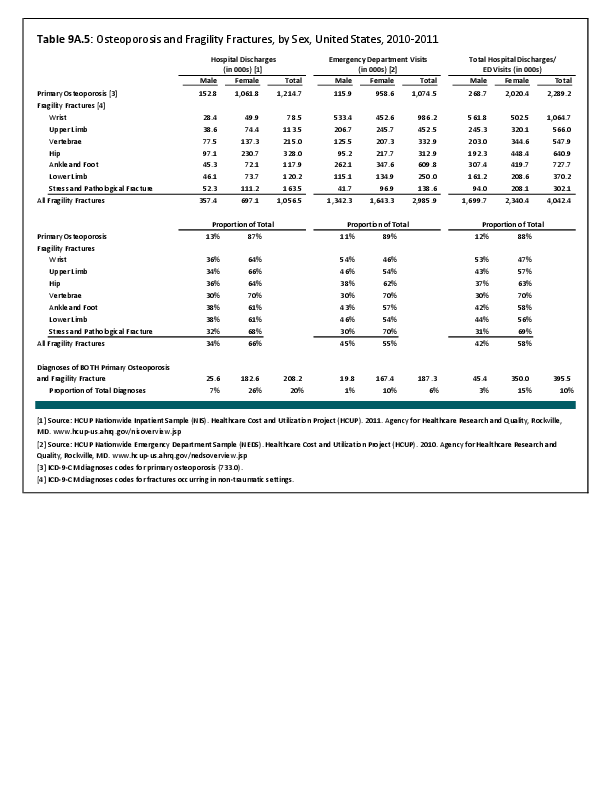
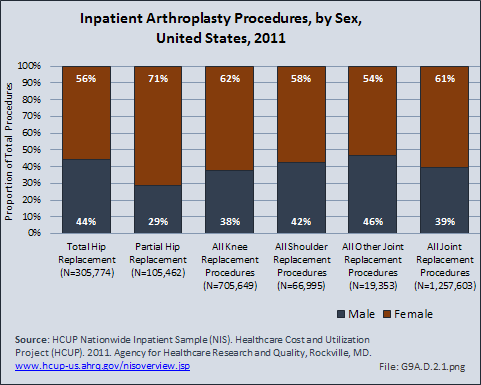
Joint replacement (arthroplasty) procedures are usually performed when osteoarthritis and associated disorders have damaged joints to a point where it is extremely painful to walk and function is impacted. However, there are no objective indications for arthroplasty. Because of the higher rate of osteoarthritis found in women than in men, women are somewhat more likely to receive a joint replacement. (Reference Table 9A.4.2 PDF CSV)
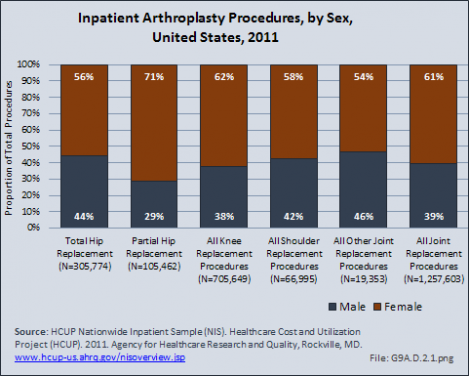
Although women receive more joint arthroplasty than do men, some studies have indicated that women are receiving arthroplasty procedures at a lower rate than anticipated, frequently reflecting the impact of gender on health.1 Hawker et al noted that women and men were equally likely to be willing to undergo arthroplasty. They also noted that women were less likely than men to have spoken to a physician regarding joint arthroplasty.1 Other studies noted that women were less likely than men to be referred by their primary care physician for consideration of joint arthroplasty, after controlling for other medical conditions.2,3 These potential delays in joint arthroplasty have significant impact. Katz et al noted that women were significantly more disabled than men by the time they underwent the procedure,4 and Ackerman et al noted that women had a significantly worse quality of life than did men during the time they were waiting for their joint arthroplasty.5 Holtzman et al noted that prior to surgery, more women than men have reported severe pain with walking, needing assistance with walking, needing help with housework, and issues walking across room or less distance; these findings were unrelated to age or comorbidities.6 Although both sexes improve when they have joint arthroplasty, some studies have indicated that women continue to have lower functional scores after surgery than men, potentially reflecting poorer function prior to the procedure and the older age of female patients undergoing arthroplasty. 7,8
- 1. a. b. Hawker GA, Wright JG, Coyte PC, et al. Differences between men and women in the rate of use of hip and knee arthroplasty. N Engl J Med 2000 April;342:1016-1022.
- 2. Rahman MM, Kopec JA, Sayre EC, et al. Effect of sociodemographic factors on surgical consultations and hip or knee replacements among patients with osteoarthritis in British Columbia, Canada. J Rheumatol 2011;38:503-509.doi: 10.3899/jrheum.100456. Epub 2010 Nov 15.
- 3. Borkhoff CM1, Hawker GA, Kreder HJ, Glazier RH, Mahomed NN, Wright JG: The effect of patients' sex on physicians' recommendations for total knee arthroplasty. CMAJ 2008 Mar 11;178(6):681-687. doi:10.1503/cmaj.071168.
- 4. Katz JN, Wright EA, Guadagnoli E, Liang MH, Karlson EW, Cleary PD: Differences between men and women undergoing major orthopedic surgery for degenerative arthritis. Arthritis Rheum 1994 May;37(5):687-694.
- 5. Ackerman IN, Graves SE, Wicks IP, Bennell KL, Osborne RH: Severely compromised quality of life in women and those of lower socioeconomic status waiting for joint replacement surgery. Arthritis Rheum 2005 Oct 15;53(5):653-658.
- 6. Holtzman J, Saleh K, Kane R: Gender differences in functional status and pain in a Medicare population undergoing elective total hip arthroplasty. Med Care 2002 Jun;40(6):461-470.
- 7. Lavernia CJ, Alcerro JC, Contreras JS, Rossi MD: Patient perceived outcomes after primary hip arthroplasty: Does gender matter? Clin Orthop Relat Res 2011 Feb;469(2):348-354. doi: 10.1007/s11999-010-1503-5.
- 8. Parsley BS, Bertolusso R, Harrington M, Brekke A, Noble PC: Influence of gender on age of treatment with TKA and functional outcome. Clin Orthop Relat Res 2010 Jul;468(7):1759-1764. doi: 10.1007/s11999-010-1348-y.
Edition:
- 2014







 Download as CSV
Download as CSV