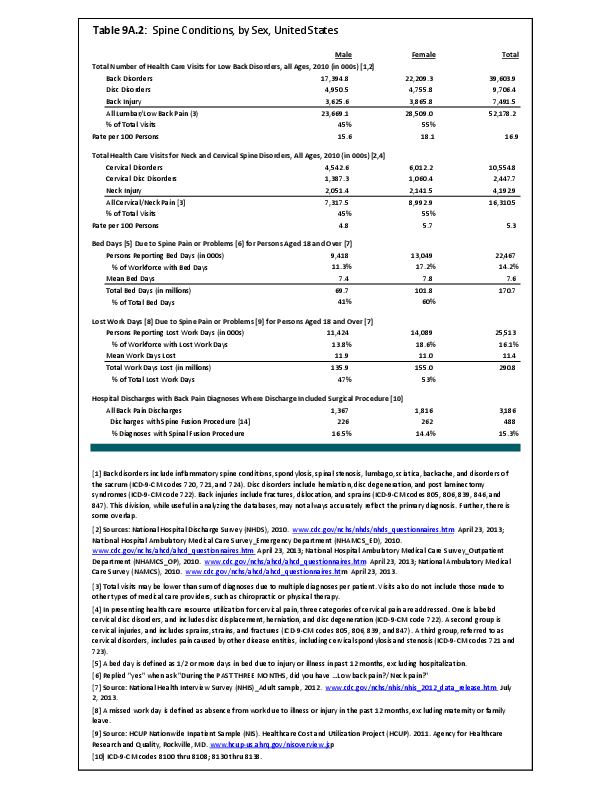
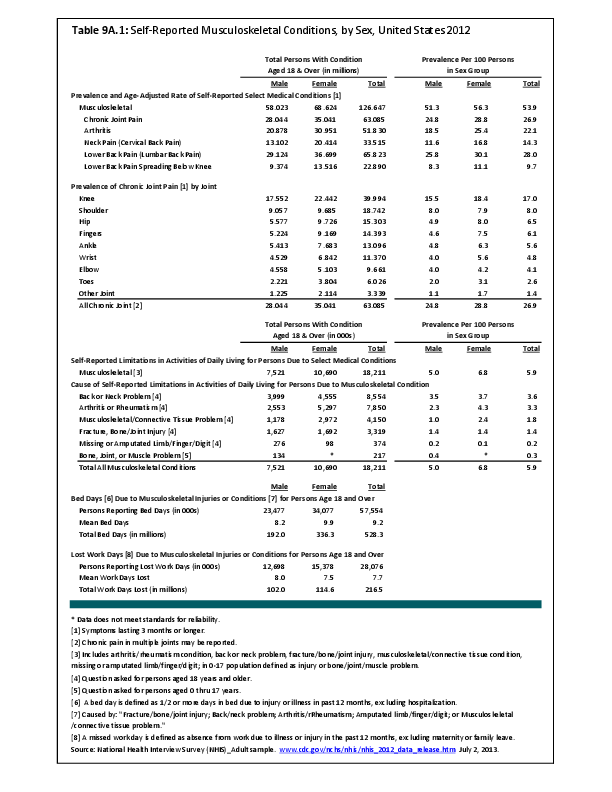
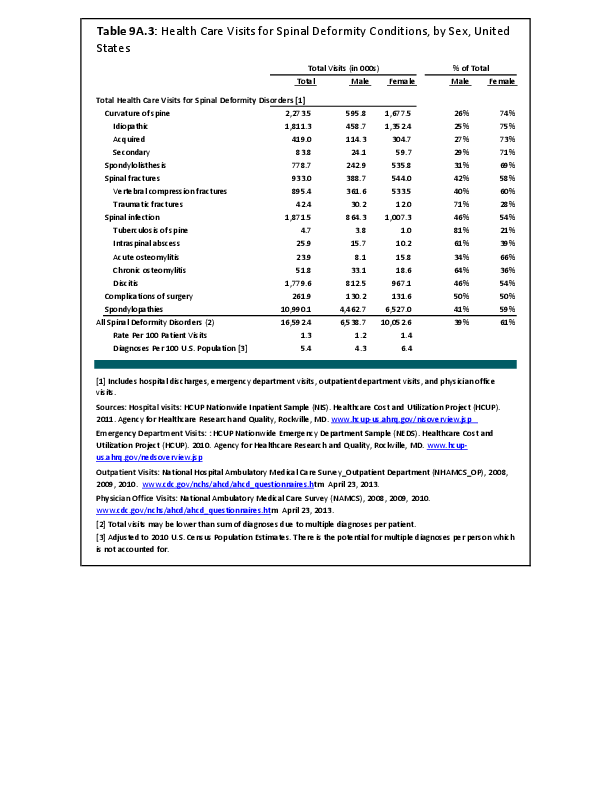
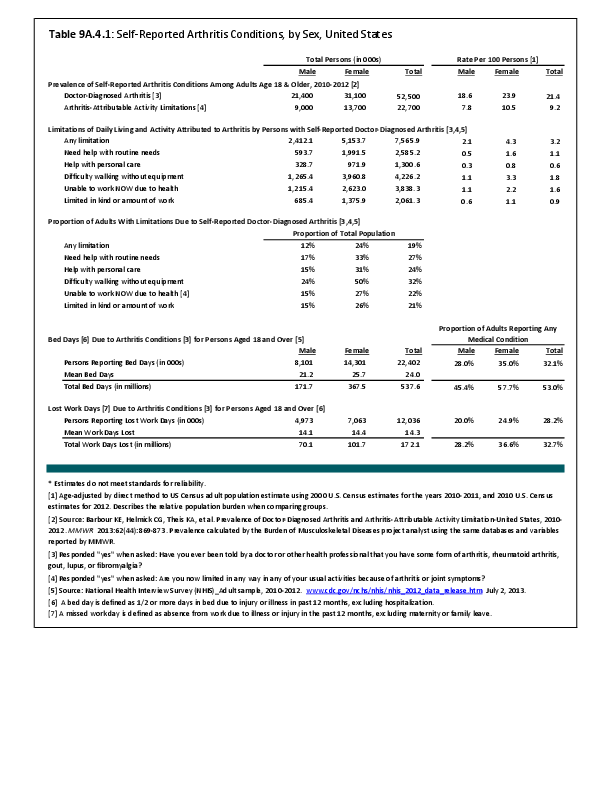
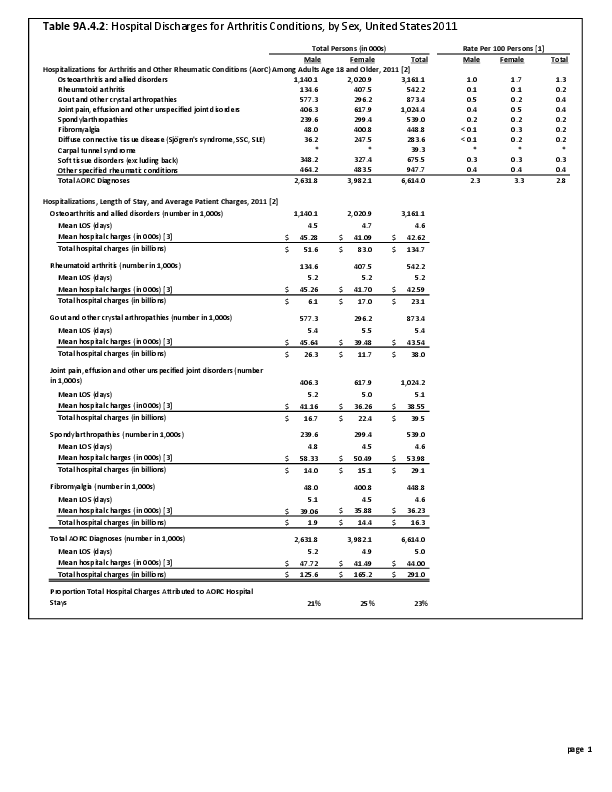
Arthritis is a condition impacted by both sex and gender. Women are more likely to present with inflammatory arthritis and osteoarthritis than are men as reflected by both self-report and radiographic studies. Specific joints appear to be at particular risk of sex-based disparities in incidence. Sodha noted in a study of hand radiographs that, after the age of 40 years, women were significantly more likely than men to have incidentally noted radiographic osteoarthritis of the hand, especially the first carpometacarpal joint.1 This incidence increased with age, especially for women, with more than 90% of women over the age of 80 years having this finding.
The increased risk of inflammatory arthritis likely reflects the overall higher rate of inflammatory conditions found in all organ systems among women. This may reflect an impact of sex hormones, especially alterations in estrogen levels, as estrogen has been found to impact B and T cell homeostasis, as well as to impact interferon regulation.2 A variety of etiologies have also been proposed, but contradictions remain in the available evidence.
The etiology of the higher rate of osteoarthritis among women also is still under debate and appears to be multifactorial. There is some indication that osteoarthritis in women has a different course than seen in men. Maillefert 3 followed 508 patients with osteoarthritis of the hip and noted that women are more likely to have polyarticular disease (pain in multiple joints), superolateral migration of femoral head, more severe symptoms, and more rapid loss of joint space. Some conditions that may increase the risk of osteoarthritis are more common, or differ in presentation in women. For example, the rates of acetabular dysplasia and pincer-type femoroacetabular impingment are higher in women. Potential explanations for differences in osteoarthritis of the knee, one of the more commonly involved joints, includes a higher lower-extremity–injury rate, differing lower-extremity alignment, lower muscle strength, and the impact of estrogen loss after menopause.
As will be discussed in another section, women are significantly more likely to sustain non-contact anterior cruciate ligament (ACL) injuries. Roos4 noted that women who had sustained an anterior cruciate ligament (ACL) injury were not only significantly more likely to have osteoarthritis of the knee than other women of the same age, they were also more likely to have osteoarthritis than men who had sustained an ACL injury at a similar age. This may reflect differing inflammatory responses at the time of injury or other factors that affect the risk of developing osteoarthritis.
Women with radiographic findings of osteoarthritis of the knee, including those without self-reported symptoms, have been noted to have weaker quadriceps than those without such changes; this relationship has not been investigated among men.5 This relative muscular weakness may translate into greater rate and degree of loading or force transmission to articular cartilage.
The impact of estrogen loss on articular cartilage and the consequent development of osteoarthritis has not been clearly defined. Estrogen receptors have been identified on chondrocytes and synoviocytes. Estrogen appears to inhibit production of matrix metalloproteinases and, thus, may help to inhibit cartilage degradation. Articular cartilage defects appear to progress more rapidly in ovariectomized (OVX) rats than they do in native rats; these defects progress more slowly in OVX rats treated with estrogen or SERMs. There are limited clinical studies in humans, and the relative impact of estrogen loss on developing osteoarthritis has not been identified. Estrogen also influences ligamentous laxity, and its loss may represent one of the many factors leading to an increased risk of osteoarthritis among women.
- 1. Sodha S, Ring D, Zurakowski D, Jupiter JB: Prevalence of osteoarthritis of the trapeziometacarpal joint. J Bone Joint Surg Am 2005;87(12):2614–2618.
- 2. Pennell LN, Galligan CL, Fish EN. Sex affects immunity. J of Autoimmunity 2012; 38:282-291.
- 3. Maillefert JF, Gueguen A, Monreal M, et al: Sex differences in hip osteoarthritis: Results of a longitudinal study in 508 patients. Ann Rheum Dis 2003 Oct;62(10):931-934. doi: 10.1136/ard.62.10.931.
- 4. Roos, M: Joint injury causes knee osteoarthritis in young adults. Curr Opin Rheumato. 2005 Mar;17(2):195-200.
- 5. Palmieri-Smith RM, Thomas AC, Karvonen-Gutierrez C, Sowers MF: Isometric quadriceps strength in women with mild, moderate, and severe knee osteoarthritis. AM J Phys Med Rehabil 2010 Jul;89(7):541-548.
Edition:
- 2014







 Download as CSV
Download as CSV