

Injuries involving the spine represent a relatively small percentage of the overall number of acute musculoskeletal injuries, but have a disproportionate impact on patient impairment, economic cost, and societal burden. These injuries encompass a wide spectrum of spinal trauma, from devastating high-energy spinal cord injuries (SCI) in younger patients that often require complex spinal reconstruction procedures to more benign low-energy osteoporotic vertebral compression fractures (VCF) in the elderly. Yet as many as 40% of patients with low energy VCF will go on to develop chronic disabling pain and deformity.1 Because spinal trauma has such a large and disproportionate impact on disability and utilization of health care resources, frequently resulting in significant structural abnormalities, we have chosen to include a focused evaluation of spinal fractures in the Deformity Chapter. High- and low-energy fractures are also discussed in the Musculoskeletal Injuries and Osteoporosis chapters, respectively. Data is derived from the various public-use databases using traumatic spine fracture injury and vertebral compression fracture codes listed at the end of this chapter.
Vertebral compression fractures are most commonly low-energy injuries that occur in patients with underlying osteopenia or osteoporosis. They affect between 700,000 and 1,000,000 persons in the US annually, and 25% of woman in their lifetime.1,2 Many low-energy fractures are treated nonsurgically with a short period of bed rest, pain medications, bracing, and therapy. Approximately 30% to 40% of patients, however, develop disabling pain and/or deformity (kyphosis), resulting in 150,000 hospitalizations annually. Frequently, patients with VCF also have reduced pulmonary function (FVC), increased risk of mortality (compared to age-matched controls), and a lower 5-year survival when compared to hip fracture patients.3 Treatment of symptomatic VCF with vertebral augmentation (vertebroplasty or kyphoplasty) has been shown in various studies to be a cost-effective intervention that both decreases pain and improves survival.4,5,6 Various strategies have been employed to prevent and treat the osteoporosis that predisposes to these “fragility fractures” and is further discussed in the Osteoporosis chapter.
Traumatic spine fractures are usually high-energy injuries that typically involve young, male patients. Most injuries are the result of high-energy falls (35% to 40%), followed by traffic accidents (20% to 30%), and low-energy falls (20% to 25%).1,2,3,4 Approximately one-half involve the thoracolumbar spine (T12–L2), while 20% involve the cervical spine. Neurologic injury occurs in 16% to 25% overall, but in as many as 40% of cervical fractures. There are approximately 12,000 spinal cord injuries each year,2,3 which are associated with a significant mortality rate. Fractures without neurologic injury generally occur three times more frequently, with an estimated 36,000 traumatic spine fractures each year. Most traumatic spine fractures are treated nonsurgically with a one- to three-month period of immobilization and bracing. Unstable fractures and those with neurologic impairment may require surgical treatment, extensive rehabilitative services, and often develop long-term disability.
Based on the HCUP Nationwide Inpatient Sample (NIS) and Nationwide Emergency Department Sample (NEDS) databases queried, there were an estimated 795,300 hospital discharges and emergency department visits for spinal fractures in 2010–/2011. Nearly three out of five spinal fractures occurred in women.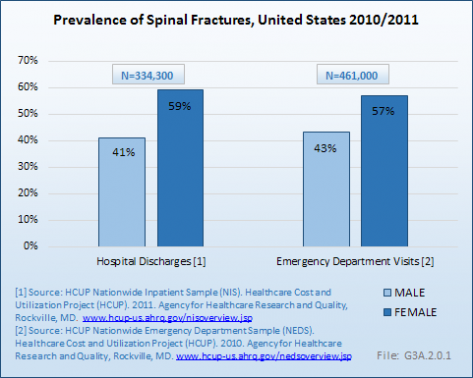
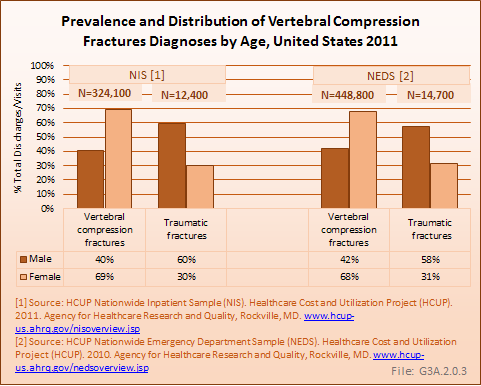
The great majority of hospital/ED combine spinal fracture patients (773,000, or 97%) were treated for vertebral compression fractures (VCF), and more than one-half (58%) involved women. Nearly half of discharges and visits for VCFs were for persons age 75 years and older.
Traumatic fractures were far less common, with 27,100 (3%) hospital discharges or outpatient visits reported in the 2010–2011 Heathcare Cost and Utilization (HCUP) databases. Numbers were too small for reliable reporting in the National Center for Health Statistics (NCHS) databases, which include outpatient and physician office visits. Traumatic fractures predominantly involve men (about 60%), and are most likely to involve patients between the ages of 18 and 44 years. These are coarse estimates, as some ED patients are admitted (samples may overlap and overestimate), while outpatient visits are not included. (Reference Table 3.1.1 PDF [2] CSV [3] and Table 3.1.2 PDF [4] CSV [5])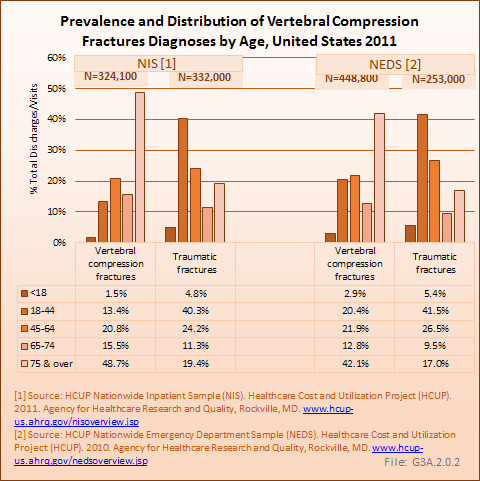
Discharge status from the hospital had a direct and linear correlation with age. For patients under 18 years of age, 72% were discharged home while only 15% were discharged to a long-term facility. The discharge status progressively changed with increasing age so that, for patients age 75 years and older, 19% were discharged home while 58% were discharged to a long-term facility. Although the overall rate of patients discharged to long-term care is slightly higher than for traumatic fractures than for VCF (54% vs. 42%), the age correlation appears to be independent of fracture severity because younger patients likely had more severe fractures. (Reference Table 3.3.1 PDF [6] CSV [7] and Table 3.3.3 PDF [8] CSV [9]) (G3A.2.1)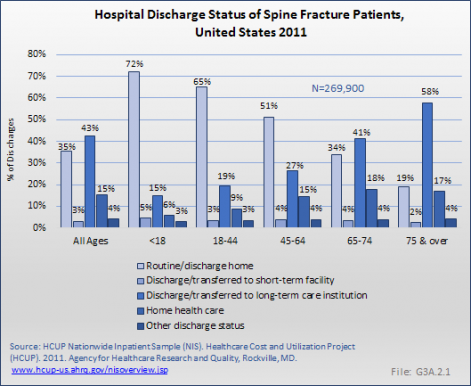
The average length of stay for those patients discharged from hospitals with a spine fracture diagnosis was 6.8 days, with an average charge of $69,500. The charges for both males and younger patients were 30% to 60% higher than the average. Similarly, the length of stay was higher in younger patients (8 days or more), and gradually decreased with age (6 days for those older than 75 years of age). This correlation most likely reflects the higher association of more complicated traumatic fractures in these younger patient populations. (Reference Table 3.4.1 PDF [10] CSV [11])
Nearly two in three patients seen in the ED with spinal fractures were transferred to a hospital. Patients admitted to the hospital from an emergency department had slightly longer average length of stay (LOS) (7.2 days) and higher charges ($70,700) than those directly admitted to the hospital. Most patients with a primary diagnosis of spine fracture admitted to the hospital from the ED were discharged to a long-term care facility (42%) and another 37% were discharged to home. The likelihood of discharge to a long-term facility was also directly related to age as noted previously. (Reference Table 3.1.2 PDF [4] CSV [5]; Table 3.4.2 PDF [12] CSV [13]; and Table 3.3.2 PDF [14] CSV [15])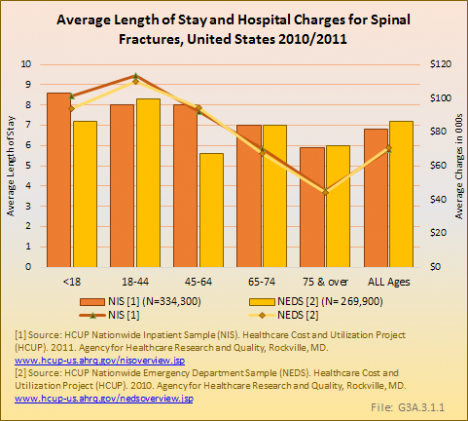
The greater severity of traumatic spinal fractures is dramatically illustrated by average hospital stays more than twice as long as for VCFs (14 days vs. 6.6 days), and average charges three times as high ($197,700 vs. $65,700). Differences in LOS and charges are particularly dramatic for persons under the age of 45 years. (Reference Table 3.4.3 PDF [16] CSV [17])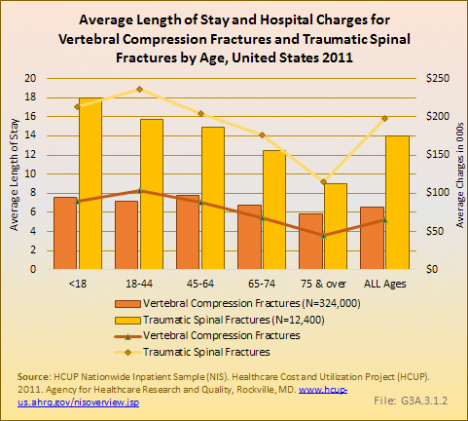
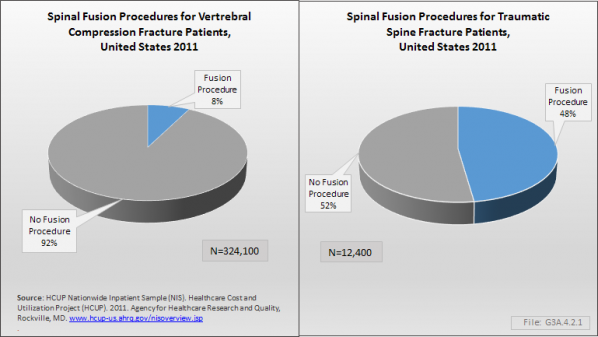
Only a small proportion of patients hospitalized with a spinal fracture undergo surgery. Of the 334,300 hospital admissions in the NIS database, fusion (8.8%) and kyphoplasty/vertebroplasty (10.6%) were the most common procedures performed. Similar rates of procedures were found in the NEDS hospitalized patients and National Hospital Discharge Survey (NHDS) databases. (Reference Table 3.5.1 PDF [18] CSV [19])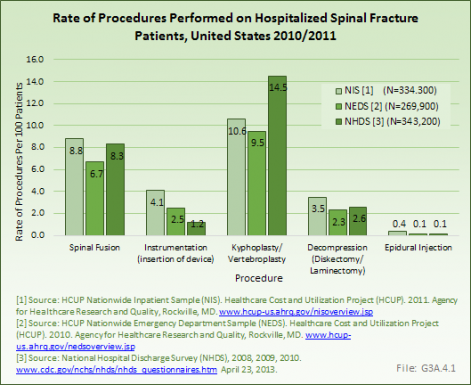
The majority of spinal fusion procedures on spine fractures were performed on patients under the age of 44 years, with patients age 65 years and older rarely undergoing surgery for spinal fractures. This is due to a much higher rate of fusion procedures performed on patients with traumatic fractures than on patients with VCFs. (Reference Table 3.5.2 PDF [20] CSV [21])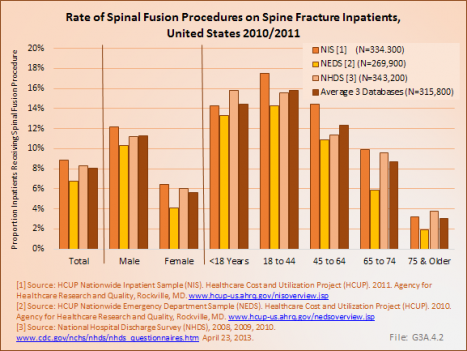
Fusions were performed most frequently in the cervical spine (41%), followed by thoracic spine (38%) and lumbar spine (26%). On average across the three databases included in the analysis, three out of four fusions performed were on four or fewer levels, with the remaining quarter of procedures involving five or more levels. (Table 3.5.3 PDF [22] CSV [23])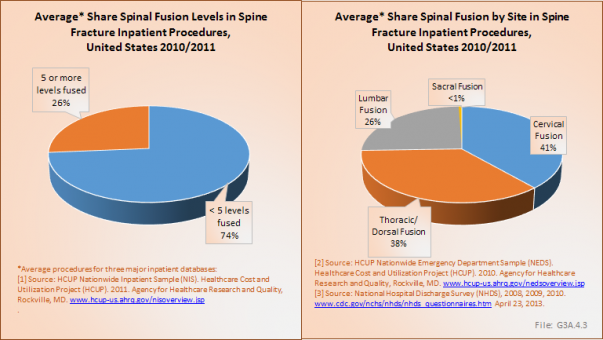
On the average, of 305,600 patients discharged with diagnosis of a vertebral compression fracture, 12% were treated with a kyphoplasty/vertebroplasty procedure. These patients were twice as likely to be female, and were most likely to be 65 or older. (Reference Table 3.5.4 PDF [24] CSV [25])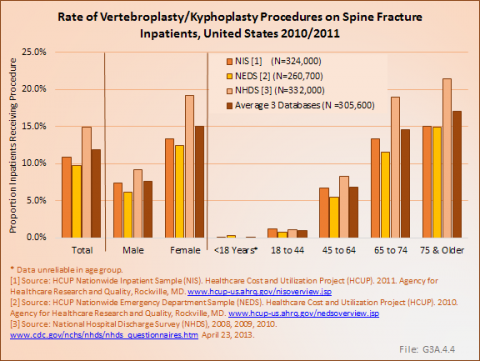
Links:
[1] http://www.spinalcord.uab.edu
[2] https://www.boneandjointburden.org/docs/T3.1.1.pdf
[3] https://www.boneandjointburden.org/docs/T3.1.1.csv
[4] https://www.boneandjointburden.org/docs/T3.1.2.pdf
[5] https://www.boneandjointburden.org/docs/T3.1.2.csv
[6] https://www.boneandjointburden.org/docs/T3.3.1.pdf
[7] https://www.boneandjointburden.org/docs/T3.3.1.csv
[8] https://www.boneandjointburden.org/docs/T3.3.3.pdf
[9] https://www.boneandjointburden.org/docs/T3.3.3.csv
[10] https://www.boneandjointburden.org/docs/T3.4.1.pdf
[11] https://www.boneandjointburden.org/docs/T3.4.1.csv
[12] https://www.boneandjointburden.org/docs/T3.4.2.pdf
[13] https://www.boneandjointburden.org/docs/T3.4.2.csv
[14] https://www.boneandjointburden.org/docs/T3.3.2.pdf
[15] https://www.boneandjointburden.org/docs/T3.3.2.csv
[16] https://www.boneandjointburden.org/docs/T3.4.3.pdf
[17] https://www.boneandjointburden.org/docs/T3.4.3.csv
[18] https://www.boneandjointburden.org/docs/T3.5.1.pdf
[19] https://www.boneandjointburden.org/docs/T3.5.1.csv
[20] https://www.boneandjointburden.org/docs/T3.5.2.pdf
[21] https://www.boneandjointburden.org/docs/T3.5.2.csv
[22] https://www.boneandjointburden.org/docs/T3.5.3.pdf
[23] https://www.boneandjointburden.org/docs/T3.5.3.csv
[24] https://www.boneandjointburden.org/docs/T3.5.4.pdf
[25] https://www.boneandjointburden.org/docs/T3.5.4.csv