

Osteoporosis can be clinically diagnosed in individuals who have had a fragility fracture, irrespective of BMD,1 particularly if the fracture occurs at the hip or spine. Fragility fractures are used to measure the burden of osteoporosis, since osteoporosis in and of itself exhibits no clinical presentations such as pain or debility.
There is no one national database that captures the number of all hip and spinal fractures and estimates how many additional people have fractures without BMD-defined osteoporosis. The Centers for Disease Control and Prevention have estimated at least 250,000 people age 65 years and older are hospitalized for hip fractures each year, using the National Hospital Discharge Survey (NHDS). Nearly all (95%) hip fractures are caused by falling, usually falling sideways.1
Another comprehensive database for evaluation of the total number of hospitalized fractures is the Agency for Healthcare Research and Quality’s (AHRQ) Nationwide Inpatient Sample [1] (NIS), and is used throughout this site to estimate burden. The NIS includes more than 8 million inpatient hospitalizations each year from all payers in the United States, and is representative of 95% of all hospitalizations in the US. Among women 55 years and older, there were almost 1.7 million hospitalizations for fragility fractures in 2011. Hip fractures were the most common (23%) fractures requiring hospitalization, representing 325,200 hip fractures. Hospitalizations for clinically evident spine fractures (8.4%), representing 245,800 patients, was the second most common type of fragility fracture. For 92% of hospitalizations for hip fracture, this was the primary, or first, diagnosis; for spine fractures, 46% were the primary diagnosis. (Reference Table 5.2.1 PDF [2] CSV [3])
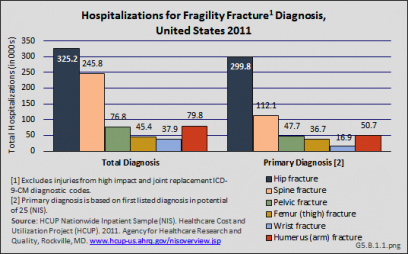
Relying on hospitalized fractures may underestimate the true prevalence of fragility fractures in the United States, since many fractures do not require hospital treatment and approximately two-thirds of all vertebral fractures are not clinically diagnosed.2 An analysis of the AHRQ NIS and National Emergency Department Sample (NEDS), and the CDC National Center for Health Statistics National Hospital Ambulatory Medical Care Survey (NHAMCS–Outpatient) and National Ambulatory Medical Care Survey (NAMCS–Physician Offices) for the years 2010 and 2011, showed 4.3 million fragility fracture visits, of which only 18% were hospital discharge visits. Wrist and arm fractures are the most likely fragility fractures to be treated outside a hospital. (Reference Table 5.2.1 PDF [2] CSV [3])
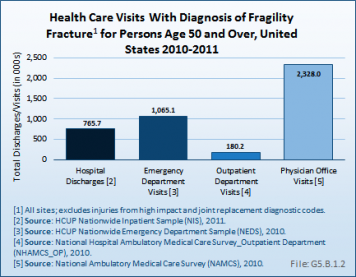
Women are more likely than men to have an osteoporosis diagnosis and to have a fragility fracture. Hospital discharges in 2011 with a fragility fracture diagnosis for women were more than twice the number of discharges in men with the same diagnosis (404,300 discharges for women; 159,500 discharges for men). This difference is evidenced for fragility fractures at all sites, and is also representative of emergency department (ED) visits with a fragility fracture diagnosis.
Age also is a major factor among people diagnosed with a fragility fracture, with people aged 80 years and older representing twice the rate of those between the ages of 70 and 79 years.
Overall, hospital discharges for fragility fractures accounted for 2.6% of hospital discharges for any diagnosis in 2011, and 2.0% of all ED visits. Among women, fragility fractures accounted for 3.5% of all hospital discharges and 2.6% of all ED visits. Among people aged 80 years and older, fragility fractures accounted for 6.4% of all hospital discharges and 4.9% of all ED visits. (Reference Table 5.2.2 PDF [5] CSV [6])
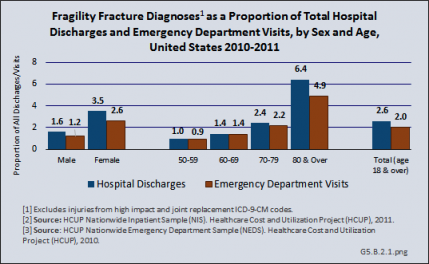
A more detailed discussion of sex and age differences in osteoporosis and fragility fractures can be found in the Special Populations section of this site in Sex and Gender [7] and Aging [8].
Although the number of hospital discharges for hip fractures has increased in recent years due to an aging population, several studies indicate a decreasing rate of hip fractures among white women and men, both in the United States and worldwide, by as much as an annualized 1.5% per year since the early 1990s.1,2,3,4,5 One recent study reports a reduction in the 10-year hip fracture probability for the white population, based on an updated study of hospital discharges using the National Inpatient Sample (NIS).6
The most recent national examination of hip fracture trends shown a decline in the age-adjusted incidence rate of fracture of 24.5% in women and 19.2% in men from 1995 to 2005.7 Racial and ethnic differences in the declines in hip fractures incidence have been evaluated. For example, a Medicare population study of hip fractures between 2000 and 2009 reported statistically significant declines in White men and women; however, due to smaller numbers, a decline among Black and Hispanic women is not statistically supported.8 Another study of hip fractures among Hispanics reported an increase in hip fractures in this population.9 Given these declines, the US version of the 10-year fracture probability calculator, FRAX, has been undated.
While declines in hip fracture incidence is being observed, fractures remain a concern because there is some indication the reduction in hip fractures is being offset with fractures in other sites, particularly vertebral fractures, due in large part to extended longevity.4
Links:
[1] https://www.hcup-us.ahrq.gov/nisoverview.jsp
[2] https://www.boneandjointburden.org/docs/T5.2.1.pdf
[3] https://www.boneandjointburden.org/docs/T5.2.1.csv
[4] http://www.cdc.gov/homeandrecreationalsafety/falls/adulthipfx.html
[5] https://www.boneandjointburden.org/docs/T5.2.2.pdf
[6] https://www.boneandjointburden.org/docs/T5.2.2.csv
[7] https://www.boneandjointburden.org/2014-report/ixae0/osteoporosis
[8] https://www.boneandjointburden.org/2014-report/ixbe0/osteoporosis-aging-population